After defects caused by tumors or infections are excluded,
skull base bone defects can be classified into two groups:
1.
CSF fistulas: when there is a communication between the intracranial and extracranial spaces.
Most bone defects are in this group.
2.
Bone defects without communications between the intracranial and extracranial spaces:
- Vascular anomalies: dehiscent carotid artery,
dehiscent high-riding jugular bulb.
- Dehiscence in the petrous portion of the temporal bone: petrous apex cephalocele,
dehiscent semicircular canal and dehiscent facial nerve canal.
1. CEREBROSPINAL FLUID FISTULAS
INTRODUCTION
A CSF fistula is a communication between the intracranial subarachnoid space and the extracranial space through an osseous or osteodural defect.
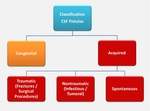
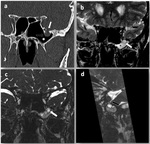
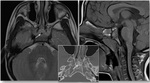
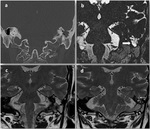
CSF fistulas can be classified as congenital or acquired.
Acquired fistulas can be classified as traumatic (caused by fractures or surgery),
nontraumatic (caused by tumors or infections),
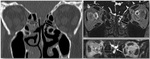
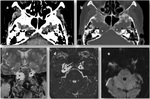
or spontaneous (Fig. 1).
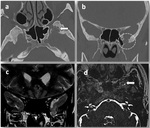
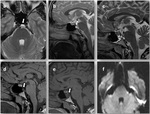
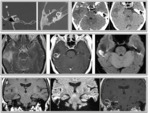
Spontaneous CSF fistulas (with no known cause):
- Most prevalent in obese middle-aged women.
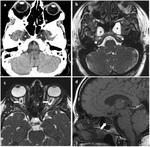
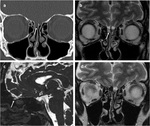
- Associated with symptoms and radiologic findings also reported for idiopathic intracranial hypertension: empty sella syndrome,
aberrant arachnoid granulations,
and other dural ectasias (Fig. 2).
- Probable etiopathogenic mechanism: failure of the arachnoid granulations to reabsorb CSF secondary to a sustained increase in intracranial pressure; the granulations enlarge and erode the adjacent bone.
If this occurs in regions with lower resistance,
especially when there is an underlying air cavity,
such as the paranasal sinuses,
it can progress with herniation of the meninges and eventually of the brain parenchyma.
- The most common locations of CSF fistulas are the cribriform plate of the ethmoid bone,
the sphenoid bone,
and the temporal bone.
CLINICAL MANIFESTATIONS
The clinical manifestations depend mainly on the location of the bone defect:
- Ethmoid and sphenoid bones: persistent rhinorrhea.
- Temporal bone: plugged filling in the ear,
otorrhea (if the eardrum is perforated),
or rhinorrhea; more rarely,
vertigo and/or tinnitus.
- Regardless of the location: epileptic seizures,
meningitis,
or other CNS infections.
DIAGNOSIS
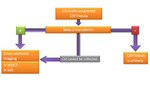
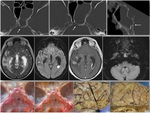
When a skull base fistula is clinically suspected,
a beta-2-transferrin (CSF-specific polypeptide) analysis in the sample of the nasal or otologic secretions should be the first test (Fig. 3).
MDCT:
- Objective: to detect the osseous defect and determine its precise location.
- Technique: multiplanar reconstructions with the bone algorithm and thin slices.
MRI:
- Objective: to evaluate the contents of a possible cephalocele,
help visualize the fistulous tract,
and rule out possible complications in the brain parenchyma.
- Technique:
· T2-weighted sequences make it possible to see the contents of the cephalocele (meningocele,
encephalocele,
or meningoencephalocele) and to evaluate possible complications in the brain parenchyma.
· CISS or FIESTA (heavily T2-weighted fast sequences) make it possible to demonstrate the CSF tract from the subarachnoid space to the extracranial space through the osseous defect.
Occasionally,
these sequences can help us to distinguish CSF from mucus in the nasal cavity and paranasal sinuses.
Here we describe the imaging findings in function of the location of the CSF fistulas.
1.1 CRIBRIFORM PLATE OF THE ETHMOID BONE
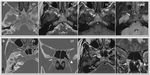
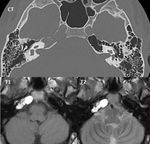
Anatomic considerations
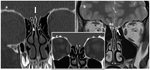
The cribriform plate is a very thin osseous structure that is sometimes difficult to appreciate even in high definition MDCT images.
It is essential to do coronal reconstructions to evaluate it correctly (Fig. 4).
Imaging findings
The cribriform plate is the most common site of CSF fistulas in the skull base.
Strong clinical suspicion is important,
because the cribriform plate is sometimes very thin and there can be false images of osseous defects.
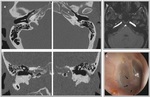
One of the CT signs that should raise suspicion of a fistula is the focal occupation of the olfactory recess,
which is a manifestation of a cephalocele (Fig. 5 and Fig. 6).
1.2 SPHENOID BONE
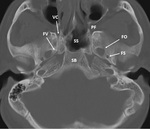
Anatomic considerations
The sphenoid bone has a complex shape.
The greater wings of the sphenoid bones have several foramina through which the cranial pairs and vessels pass to the extracranial spaces,
and it is important not to mistake these for pathologic osseous defects (Fig. 7).
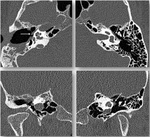
Imaging findings
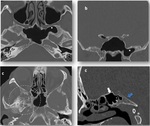
The most common locations of osseous defects in the sphenoid bone:
- Greater wings: fistulas are more common in the posterosuperior wall of the lateral recesses.
· Spontaneous fistulas occur when pneumatization of the pterygoid processes,
a normal variant,
coexists with aberrant arachnoid granulations in the wings of the sphenoid (Fig. 8,
Fig. 9,
Fig. 10 and Fig. 11).
· There are some lesions in the pterygoid processes of the sphenoid bone that should not be mistaken for bone defects.
(Fig. 12).
> Arrested pneumatization (anatomic variant): a nonexpansile lesion with a thin cortical margin,
internal fatty content,
and curvilinear internal calcifications.
> Intraosseous lipoma: radiologically can be indistinguishable from arrested pneumatization,
although it may rupture the adjacent bone cortex.
The internal calcifications can be curvilinear or coarse.
- Perisellar region (Fig. 8):
· Roof of the sphenoid sinus
· Floor of the sella turcica. Apart from the mechanism related with intracranial hypertension,
fistulas in this location can be due to the persistence of the craniopharyngeal canal,
an osseous defect in the midline of the body of the sphenoid bone,
which extends from the floor of the sella turcica to the nasopharynx.
Canals measuring a few millimeters in diameter are usually incidental findings without accompanying symptoms (Fig. 13).
Larger canals can be filled (meningoencephalocele,
tumors) and may be associated with structural malformations.
· Posterior wall of the body of the sphenoid bone (the site of the spheno-occipital synchondrosis in children).
Ecchordosis physaliphora can simulate a fistula in the posterior wall of the sphenoid sinus on CT (Fig. 14).
- Definition: a benign congenital lesion derived from the remnants of the notochord,
normally located in the retroclival prepontine region.
- CT findings: osseous defect with sclerotic margins in the posterior wall of the clivus,
with benign characteristics.
- MRI findings: the soft-tissue components can be seen with nonspecific radiologic characteristics: hyperintense in T2-weighted images,
hypointense or isointense in T1-weighted images,
and generally without contrast enhancement.
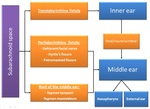
1.3 TEMPORAL BONE
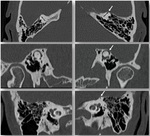
Anatomic considerations
It is essential to know the structures of the middle ear and of the internal ear,
as well as their anatomic relations (Fig. 15).
Imaging findings
CSF fistulas in the temporal bone communicate with the middle ear cavity (Fig. 16).
- Tegmen tympani and tegmen mastoideum: the most common locations in the temporal bone (Fig. 17 and Fig. 18).
Possible origin of spontaneous fistulas: congenital dehiscence or thinning of the bone and progressive erosion due to the aberrant arachnoid granulations.
Prominent granulations in this location,
even without a fistula,
are considered a predisposing factor for infections of the central nervous system (Fig. 19).
- Labyrinthine fistulas: these are uncommon congenital lesions.
The absence of the modiolus of the cochlea and a defect in the oval window allow the CSF to pass from the inner ear canal to the middle ear cavity through a dysplastic labyrinth.
- Perilabyrinthine fistulas: communications between the subarachnoid space and the middle ear through routes other than the cochlear labyrinth,
in other words,
through conducts present in the normal anatomy that have become dysplastic and can act as CSF fistulas:
· Facial nerve canal: when the labyrinthine segment of the canal and geniculate fossa are widened and dehiscent,
it could act as a fistula and debut with otorrhea.
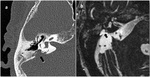
· Tympanomeningeal fissure (Hyrtl’s fissure): located below the round window and extending along the lower margin of the cochlea,
this fissure communicates the hypotympanum with the fossa posterior.
It normally ossifies between 24 and 26 weeks in utero,
but can occasionally persist into adult life,
remaining clinically silent or causing a CSF fistula.
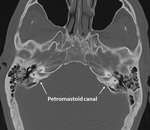
· Petromastoid canal: this canal joins the posterior cranial fossa with the ethmoid air cells and the mastoid antrum.
It courses under the arch of the superior semicircular canal and contains the subarcuate artery and vein (Fig. 20).
It has been proposed as a possible cause of CSF leakage,
but this theory is controversial.
2. NON-COMMUNICATING BONE DEFECTS
2.1 Petrous apex cephalocele
This benign cystic lesion in the petrous apex,
which can be unilateral or bilateral,
is a meningocele or arachnoid cyst originating in the posterolateral wall of Meckel’s cave.
Differential diagnosis: cholesterol granuloma,
mucocele,
cholesteatoma,
and petrositis.
Petrous apex cephaloceles are usually asymptomatic and found incidentally.
CT findings: osseous defect in the medial portion of the petrous apex.
Occupation of the middle ear or ethmoid cells is uncommon; when present,
an infection should be suspected.
MRI findings: a cystic lesion (hypointense in T1-weighted sequences and hyperintense in T2-weighted sequences) that communicates with Meckel’s cave.
Diffusion-weighted sequences help to rule out a cholesteatoma and thus avoid unnecessary surgery (Fig. 21).
Although cholesterol granulomas can be impossible to distinguish from cephaloceles on CT images,
their characteristics on MRI and their location are specific: a lesion that is hyperintense in both T1- and T2-weighted sequences without restriction in diffusion-weighted sequences.
Peripheral enhancement after intravenous contrast administration is easier to appreciate on CT than on MRI (Fig. 22).
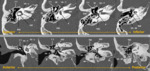
2.2 Superior semicircular canal dehiscence
Focal bone dehiscence in the roof of the superior semicircular canal.
The dehiscence creates a “third window” (in addition to the oval window and the round window) into the inner ear that is sensitive to changes in pressure and sound,
resulting in the flow of endolymph inside the semicircular canal.
This gives rise to vestibular (vertigo and/or nystagmus) and auditive symptoms (decreased hearing) induced by loud noises .
MDCT: thin slices,
obtaining axial and coronal images (Fig. 23).
Oblique images should be obtained if there are doubts.
MRI has a high negative predictive value,
so some authors propose its use as the first imaging study in patients with vestibulocochlear symptoms.
However,
its positive predictive value is relatively low,
so CT is necessary when there is strong suspicion of superior semicircular canal dehiscence.
The best sequences are fast heavily T2-weighted sequences (CISS or FIESTA),
which make it possible to visualize very small fluid-filled structures and to make multiplanar reconstructions.
2.3 Facial nerve canal dehiscence
In normal conditions,
the tympanic segment of the facial nerve courses posteriorly in the horizontal plane,
passing between the oval window and the lateral semicircular canal.
The bone lining the tympanic portion of the canal can be very thin and dehiscent.
Its course can even pass through the middle ear cavity,
thus making the nerve more vulnerable to acute and chronic infectious processes or surgical maneuvers in the area,
with possible peripheral facial paralysis in both cases.
Facial nerve canal dehiscence is more common in patients with cholesteatomas,
so it is especially important to mention it in radiology reports before surgical planning (Fig. 24).
Unlike dehiscence of the labyrinthine segment,
CSF leaks do not usually occur.
2.4 Aberrant internal carotid artery with canal dehiscence
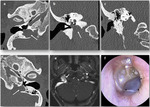
Aberrant internal carotid artery is an anatomic variant in which there is a collateral artery that became enlarged due to involution of the normal cervical portion of the internal carotid artery during embryological development.
Otoscopy shows a red retrotympanic mass,
which could be mistaken for a paraganglioma.
Imaging tests are essential to avoid biopsies that can have fatal consequences for the patient.
On CT images,
the carotid canal can be identified in the middle ear cavity,
where it courses anteroposteriorly,
with bony lining.
The aberrant artery usually has a smaller diameter than a normal internal carotid artery (Fig. 25).
CT angiography or MR angiography can help identify the exact course of the artery and thus confirm the suspected diagnosis and rule out a tumor.
The most common clinical manifestations are pulsatile tinnitus and hearing loss.
2.5 Dehiscent jugular bulb
This consists of the absence of the sigmoid bone plate that normally separates a high-riding jugular bulb from the middle ear cavity.
Otoscopy shows a blue retrotympanic mass that could be mistaken for glomus.
It enlarges with the Valsalva maneuver or jugular vein compression.
As in aberrant internal carotid artery,
biopsy can have disastrous consequences.
MDCT is the best diagnostic technique to confirm the bone dehiscence.
CT angiography can confirm that this is a vascular structure.
Dehiscent jugular bulb can be associated with another variant,
jugular bulb diverticulum,
which is defined as a polypoid extension that protrudes toward the temporal bone (Fig. 26).
MRI is usually less useful in the diagnosis of dehiscent jugular bulb.
It can help to rule out tumors as the cause of the bone defect.
MR angiography can be used instead of CT angiography.
Although variants of the jugular bulb have been associated with pulsatile tinnitus,
this association is controversial,
considering that it is a frequent finding in asymptomatic patients.
Therefore,
in patients with tinnitus and dehiscent jugular bulb,
it is important to thoroughly rule out other possible causes before reaching the definitive diagnosis.